Goals and Objectives of a Clinical Skills Lab
What is a Clinical Skills Lab?
A clinical skills laboratory (or skill lab) is an educational facility which gives students, physicians, nurses, and other healthcare professionals the opportunity to learn relevant clinical and communication skills and build competency in them before transitioning to the real hospital setting with direct patient contact.
Why do we need a Clinical Skills Lab?
In many professions around the globe, students in colleges and universities learn a comprehensive amount of information. But it is not until they step out into the real world and get a job that they begin to learn the necessary skills needed to do their job. But it is not like this in the medical profession. Whether you are a doctor, a nurse, or a tech assistant, you need to know what you are doing. You cannot risk practicing on real patients and put their lives in danger or make them uncomfortable. You cannot jeopardize their safety and create a breach of their privacy.
In fact, the majority of mistakes (and serious mistakes) happen in the first few working years after licensure, and can be chalked up to a lack of experience. After years of theoretical learning, students are given a relatively short amount of time to acquaint themselves with the practical reality of the clinical setting. Before these labs came into existence, the acquisition of these relevant clinical skills depended on appropriate patient encounters and well-trained lecturers. Today, even the ratio of the number of students to the number of teachers is off. And with the amount of technical innovations in diagnosis and treatment, it becomes all the more important to incorporate skill labs to build skills in the learners.
A clinical skills lab is able to provide a controlled, safe, forgiving environment for creating realistic, hands-on, diverse learning experiences. It’s not the same as practicing on real patients, but it’s the next best thing. Apart from clinical skills, it helps build communication skills, cognitive skills, and a compassionate approach to patient care.
A clinical skills lab usually has a reception area, skill studios, an ICU simulation room, an operation theatre simulation room, a pediatric ICU simulation room, AV facilities in the rooms, surgical simulation suites, ultrasound training rooms, seminar halls, a board room, faculty lounges, a student lounge, and necessities like storage, safety systems, and HVAC. Personnel in attendance may include a chief coordinator, supporting departmental staff, nursing staff, a receptionist, and a biomedical engineer.
Goals and Objectives of a Clinical Skills Lab
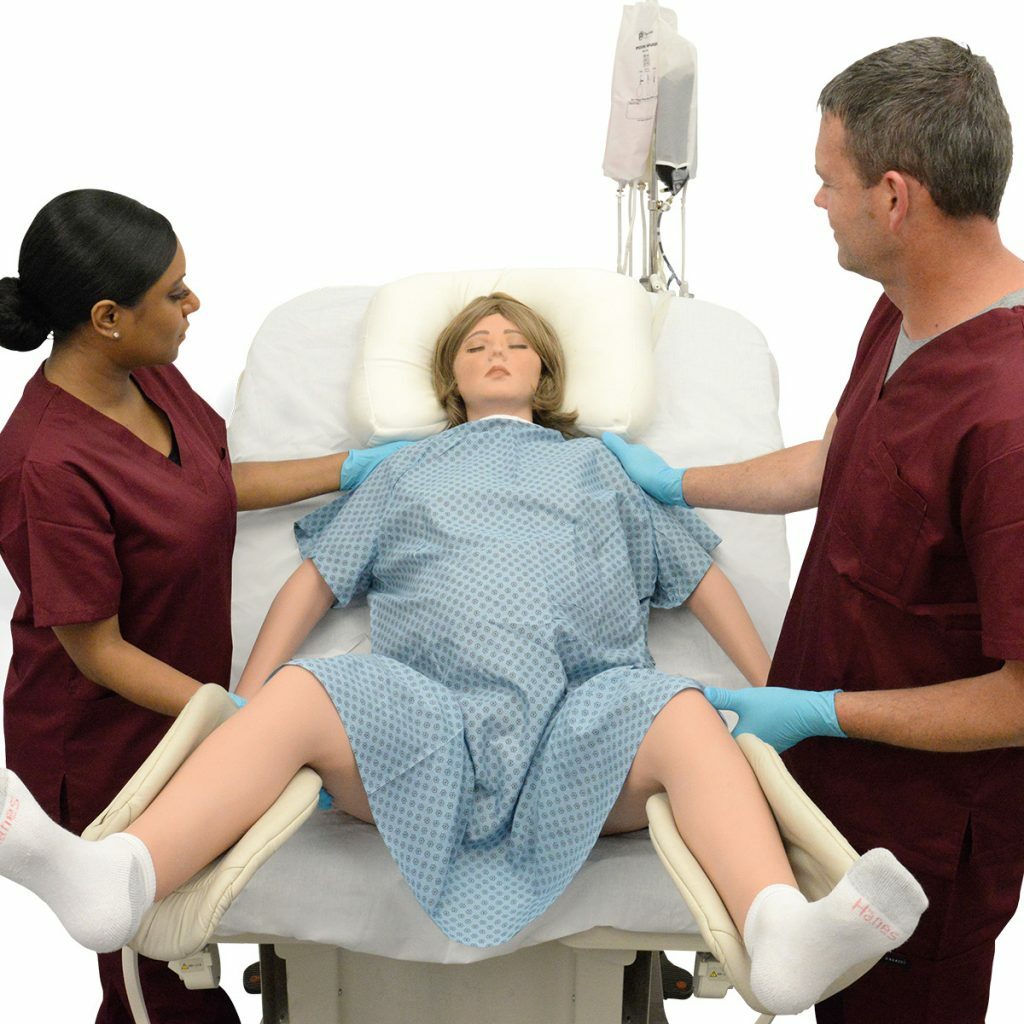
- To encourage and support learning through simulation technology and simulators, manikins, and trainers.
- To provide a safe platform for hands-on learning experiences in order to build relevant clinical skills.
- To provide a controlled, anxiety-free, and risk-free learning environment to students.
- To provide a platform for repeated practice for mastery in relevant clinical skills – for novices and experts alike.
- To build a strong foundation of the fundamentals in the learners.
- To accommodate the unique learning needs of students with diverse backgrounds, abilities, and educational experiences.
- To provide educational materials for students, faculty, and staff of medical and nursing colleges.
- To encourage a life-long learning model.
- To make sure to include all environmental factors and make the learning experience as realistic and authentic as possible.
- To integrate clinical simulation into medical and nursing curricula.
- To increase the preparedness of student learners before transitioning to the real hospital setting.
- To increase their preparedness for dealing with high acuity cases.
- To build strong communication skills.
- To enable learners to think on their feet.
- To enable learners to make critical decisions.
- To ensure adaptation of best practices in the industry
- To prepare students to be able to handle emergency situations
- To encourage and demonstrate the power of team-building and collaboration.
- To build problem solving and decision-making skills through simulations and case scenarios.
- To provide learners with debriefing and positive feedback of their performance.
- To provide learners with real-time feedback through simulator screens, allowing them to reflect and use critical thinking during the process.
- To build dexterity in various clinical skills like examination, diagnostic reasoning, communication, and execution of clinical techniques.
The purpose of clinical skills lab or simulation-led medical education is not to replace traditional teaching methods, but to complement them. Over the years, these labs have come to be widely accepted as an essential part of medical education and colleges, and have helped numerous learners become job-ready in the medical industry, proving to be an indispensable asset to the industry.
More Blog:
How to use the 3b Scientific p90 Birthing Simulator by SEM Trainers?
Follow us on Social Media :